- What is Naviguard?
- Where Naviguard fits in the healthcare benefit process
- How we can help resolve out-of-network medical bills
We know how it feels to get an unexpected medical bill — scary
It’s happened to so many of us: you get a medical bill that throws you for a loop. It’s from a provider that’s out-of-network — not on your plan’s list of in-network providers.
You feel your blood pressure rising. It’s frustrating, because you may not have even known you went outside your plan’s network. Maybe you had a procedure that involved various services and included a provider you didn’t know was out-of-network. Or maybe you were just following a recommendation of your in-network provider.
Worse yet, there’s the bill with that big number and dollar sign in front of it. Facing an unexpected out-of-network balance medical bill can be terrifying. In fact, many people say getting the bill was more traumatic than the medical event itself. How will you possibly afford it? What do you do next?
Don’t panic, and don’t pay your medical bill yet
Most people aren’t familiar with how to negotiate out-of-network balance medical bills. Naviguard® was created for exactly this situation and exactly this purpose: to help members deal with unexpected, out-of-network balance medical bills. Our goal is to provide clarity and help reduce the costs when appropriate.
We do this by making sure you’ve actually been billed correctly, by making sure your benefits were applied correctly and — this is the big one — by negotiating with providers on your behalf for a lower bill when appropriate.
Resolving issues around out-of-network balance medical billing is Naviguard’s primary focus. We know how shocking it can be to get a big medical bill, and you shouldn’t have to face it alone. If your UnitedHealthcare plan includes Naviguard, our services are available to you at no additional cost. By managing all the details and the interactions with providers, Naviguard can help you breathe a huge sigh of relief.
We can help make sure you pay an appropriate amount
Naviguard has experts who bring a deep understanding to your situation, along with decades of health care and health insurance experience. We know the provider networks well and have access to the most up-to-date industry pricing.
That means we know what providers should be charging for the services you received, in the area where you live. This knowledge arms us with the information we need to effectively negotiate more appropriate rates on your behalf.
Because the resources we use are widely accepted and the numbers we reference are based on local market rates, we can negotiate from a position of strength. We’re often able to arrive at an acceptable compromise quickly.
Naviguard’s track record of success
Our experts have helped tens of thousands of members navigate difficult balance medical bills with significant success. This includes more than 350,000 cases, engaging with more than 5,900 providers across the U.S. in over 170 specialties.*
While we work on behalf of our members and promise our full support in resolving issues for you, we aim to make the process straightforward, easier, and fair for everyone involved — members, employers and health care professionals.
How Naviguard may be able to help you
Naviguard provides flexible options to help resolve out-of-network balance medical bills — from dedicated one-on-one service by a personal advisor to digital self-service resources. Naviguard.com is a great place to start.
Here are some of the key ways Naviguard may be able help you:
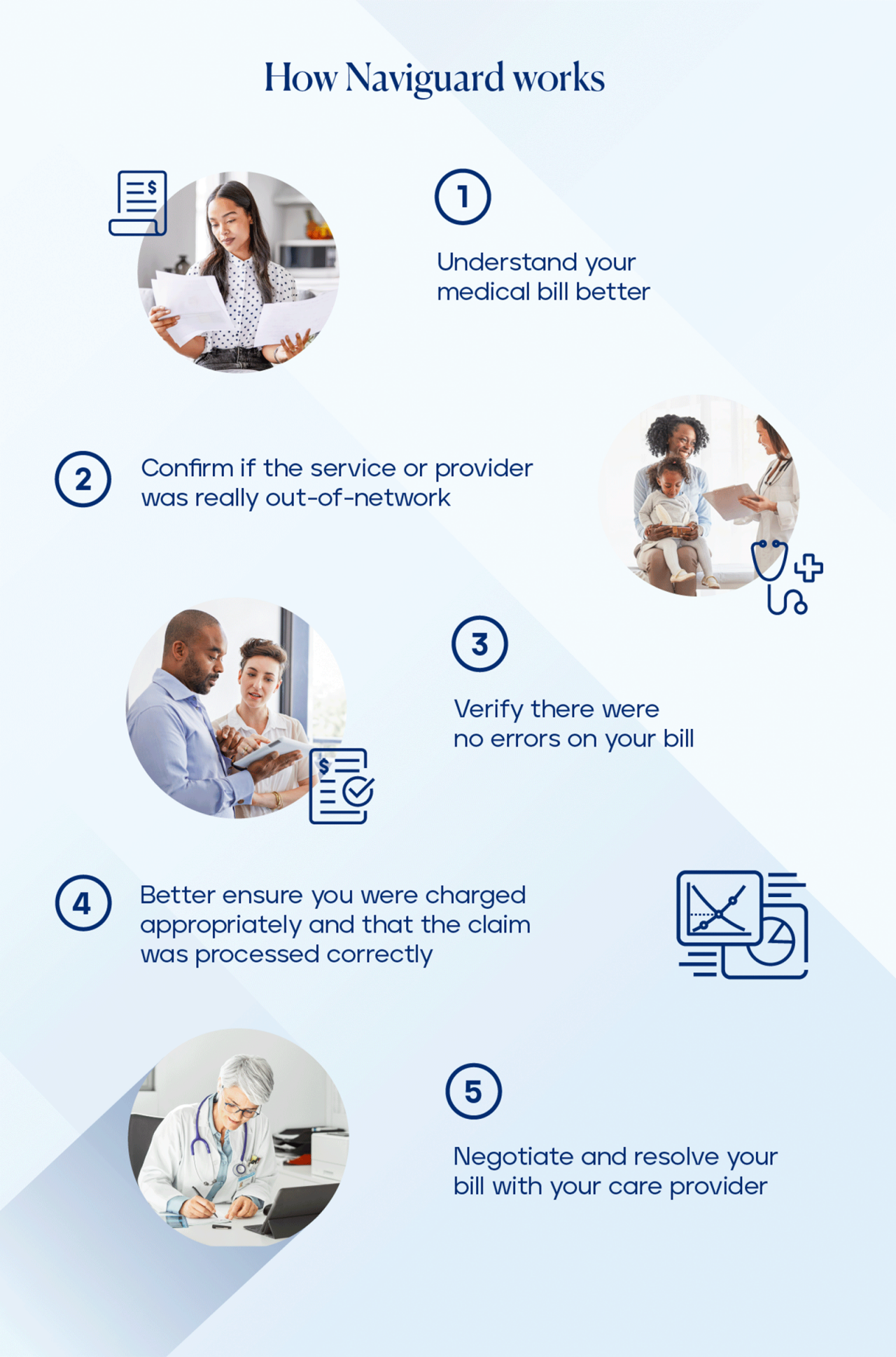
It’s not a one-size-fits-all process
Unexpected out-of-network balance medical bills have arrived in the mailbox of nearly half of all Americans, yet every circumstance, and every member, is different.
We believe better information leads to better outcomes, which is why we tailor our approach to your situation. We help strengthen your case by understanding and including details of your specific story and using them as part of our negotiating strategy.
Naviguard: here through thick and thin
When an unexpected out-of-network balance bill arrives, it’s comforting to know you’ve got someone in your corner. Someone who can bring clarity and resolution when it’s needed most. Someone with experience, expertise, and a lot of past success in managing challenges just like yours, and not at all like yours. That someone is Naviguard. And we’re ready to go to work for you.
To learn more about the services we offer, talk to your employer, or contact us today.
*Based on Naviguard’s engagement with its members from January 2021 through October 2023.
RESOURCES

